Microvascular Free Tissue Transfer Has Become Gold Standard for Complex Head and Neck Reconstruction
“In the last 15 years, head and neck microvascular reconstruction has become the gold standard for any complex reconstruction,” said Yash J. Patil, MD, associate professor of otolaryngology, and director of the adult airway reconstruction program, University of Cincinnati (UC) Medical Center. According to Dr. Patil, who initiated the microvascular program at UC Medical Center and earlier at the University of South Florida, mechanical venous anastomosis in head and neck microvascular reconstruction allows surgeons to “quickly and effectively” treat patients with complex conditions. During the procedure, surgeons transfer tissue (skin, bone, nerves or a combination) from other parts of the body and attach it to the part of the head or neck from which the tumor has been removed.
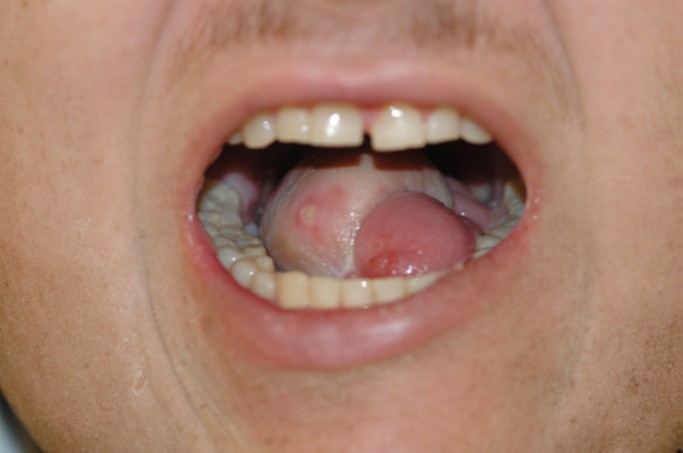
This patient received replacement of more than half of his tongue with free flap reconstruction. Following the procedure, the patient was able to speak and eat normally. Image courtesy of Yash Patil, MD.
Free tissue transfer has several advantages, according to Dr. Patil: “we bring new tissue to the defect to recreate bone or skin and preserve form and function, as much as we can; it allows us to remove the cancer to the fullest extent possible; and the patient experiences quicker healing with fewer complications than is usually seen with the older skin grafting and suture technique.” Discussing the flexibility and durability of free flaps, also known as free autologous tissue transfer or microvascular free tissue transfer, Dr. Patil observed that “the head and the neck are often the most difficult sites to heal, with very thin tissue that breaks down with radiation or chemotherapy. However, free flap reconstruction provides thick, well-vascularized muscle or skin or healthy bone. Our success rate is very high – 95% to 98% of our patients heal.” In a retrospective study published this year by Thorne and Patil, flap survival exceeded 98% in 402 patients and 431 total microvascular free flap reconstructions over eight years.1
Removal of the cancerous tumor and reconstruction are done at the same time; these two surgeries take a total of “4 to 6 hours, considerably less time than in other institutions because of UC Medical Center’s high-volume efficient system,” said Dr. Patil. UC Medical Center’s streamlined process includes an ENT team and an OR, both dedicated to microvascular reconstruction, with an anesthesiologist and an intensivist similarly assigned. “We have established clinical care pathways that provide continuity of care for our patients; we study these pathways so that patient care is modifiable and reproducible,” said Dr. Patil, estimating that the UC Medical Center group that he directs has performed about 150 flap procedures in the last year.
Reference
1. Thorpe E, Patil Y. Mechanical venous anastomosis in head and neck microvascular reconstruction as an equivalent to the gold standard. Ear Nose Throat J. 2017;96(2):E32-E36.
Yash J. Patil, MD
Associate Professor of Otolaryngology
Director, Adult Airway Reconstruction Program, University of Cincinnati Medical Center
Phone: (513) 584-2003
Email: patilyj@ucmail.uc.edu
Connect with Dr. Patil on Doximity
Leave a reply →

