New Surgical Skills Laboratory to Provide Residents Critical Skills for Real-Life Scenarios
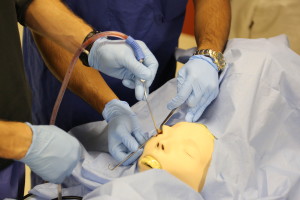
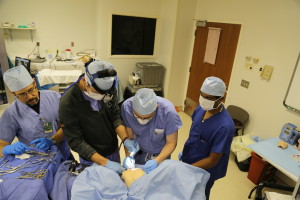
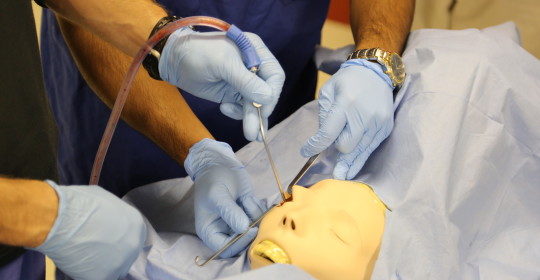
Surgical simulation has emerged as a proven training tool with significant potential for refreshing previously acquired skills and learning more advanced procedures and techniques.1 As surgical simulation technology has evolved, one of its earliest users, the University of Cincinnati Medical Center has kept pace with these changes. The UC Medical Center Department of Otolaryngology – Head and Neck Surgery has a long history of using simulation for training, from its early temporal bone laboratory to its current Resident Bootcamp and Midwest Airway course, and the newest expansion of this initiative is a state-of-the-art Surgical Skills Laboratory. The Surgical Skills Laboratory, which is currently under construction and expected to open within the next year, will be available 24/7 and provide critical skills training to all otolaryngology residents in both the adult and pediatric programs.
Charles M. Myer, IV, MD, head and neck surgeon at Cincinnati Children’s Hospital Medical Center who leads this initiative, explains, “The goal of simulation is to provide opportunities for residents to practice in real-world situations without risk to the patient.” Faculty will conduct lectures and workshops in the Skills Laboratory, as well as review videos of the residents performing specific skills to evaluate their competency. Helping residents develop the “muscle memory” necessary to perform both common and uncommon procedures, the Surgical Skills Laboratory will be especially useful in providing an opportunity to practice working with high-risk, low-frequency conditions such as orbital hematomas, thyroid hematomas, and airway foreign bodies.
Zenker’s diverticulostomy is one example of a procedure that residents will be able to practice before encountering it in the operating room. Myer and his colleagues have submitted for publication their experience with modifications made to a Zenker’s simulator to improve the fidelity and use as a standardized competency assessment tool.2
In the past, University of Cincinnati Medical Center utilized an apprenticeship model with new residents learning by “shadowing” more experienced clinicians, gradually performing more arduous tasks. However, work hour restrictions have made that approach increasingly difficult. In addition to decreased fatigue and improved functionality among residents, it also contributed to an environment where these trainees have fewer opportunities to practice common procedures and less exposure to more uncommon conditions. The Surgical Skills Lab seeks to respond to this evolving training environment. “Having this space will allow us to move forward and improve our simulation-based education,” concludes Myer. “The role of medical simulation is very innovative and I believe we’re on the cusp of a paradigm shift with academic medical centers starting to embrace this new learning technique.”
References: 1. Heskin L, Mansour E, Lane B, Kavanagh D, Dicker P, Ryan D et al. The impact of a surgical boot camp on early acquisition of technical and nontechnical skills by novice surgical trainees. Am J Surg September 2015;210(3):570–577. 2. Richtsmeier WJ. Simulated Zenker’s endoscopic staple-assisted esophagodiverticulostomy (ESED) surgery. Laryngoscope. 2002 Jul;112(7 Pt 1):1230-4.

Charles M. Myer, IV, MD
Department of Otolaryngology – Head and Neck Surgery
Cincinnati Children’s Hospital Medical Center
Phone: (513) 636-4355
Email: charles.myer@cchmc.org
Connect with Charles Myer, IV, MD on Doximity