Pediatric Voice: Improving Voice While Maintaining Good Breathing
At the beginning of the pediatric voice program at the University of Cincinnati (UC) Medical Center, “we were satisfied with successful airway reconstruction in our patients that allowed them to have some voice,” says Alessandro de Alarcon, MD, MPH, UC Health. Over the last 10 years, UC Medical Center has become concerned with assessing the quality of pediatric patients’ voices as they grow, including soft/weak voices and other voice problems that can be improved and treated. “Patients who have had complex surgery for breathing now want to address these issues, and we want to make their voices better without worsening their breathing. Maintaining this balance has become our expertise,” explains Dr. de Alarcon, associate professor, otolaryngology-head and neck surgery, and director, Center for Pediatric Voice Disorders, UC Medical Center/and Cincinnati Children’s Hospital Medical Center.
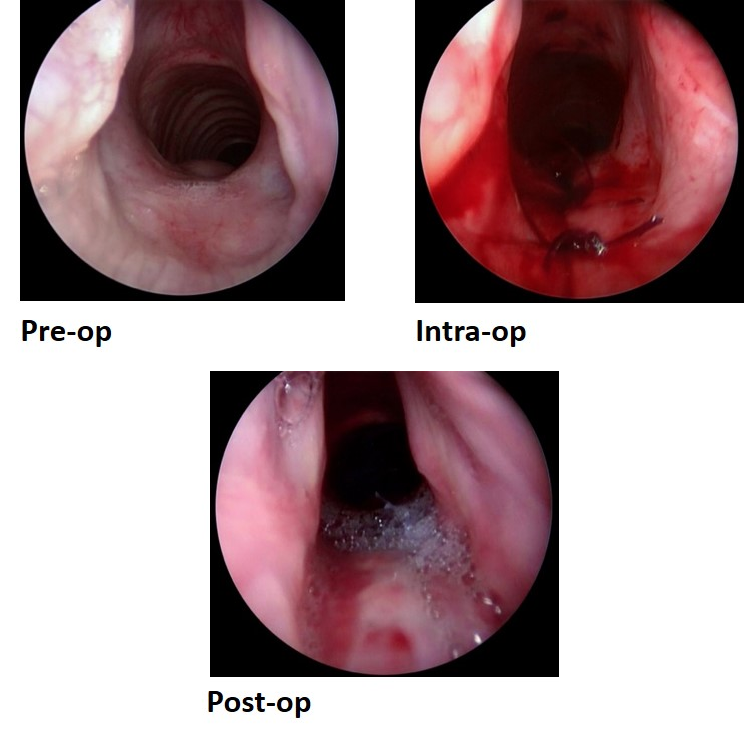
The above images show endoscopic posterior cricoid reduction in the pre-op, intra-op and post-op stages. Images courtesy of Alessandro de Alarcon, MD, MPH.
The first step, evaluating voice problems, has been aided by the development of new tools, such as laryngeal high-speed videoendoscopy (HSV) and dynamic voice computed tomographic (CT) scans. “High-speed videoendoscopy provides us with views of the laryngeal structures at very high speeds, frame rates of 8,000 to 10,000 frames/second, which gives us a better understanding of some of these very abnormal voices, especially those not created from vocal cords, but from other structures such as supraglottic sources, the lower pharynx or the upper esophagus,” Dr. de Alarcon says. That has led to ongoing collaborations with colleagues at Michigan State University. “Dimitar Deliyiski, PhD, at Michigan State is the leader in HSV technology and together we are better trying to understand the mechanisms of voicing that occur in these patients as well as which patients are most at risk,” Dr. de Alarcon says. UC Medical Center physicians also want to identify those who will have a voice problem, and what type of problem, before airway reconstruction is performed. “We want to be able to tell the patient and parents/caregivers what kind of voice they can expect. Many institutions aren’t thinking this way yet. UC Health, with close to 40 years of performing airway reconstruction, sees this as a critical best practice,” Dr. de Alarcon says. “I am collaborating with my adult laryngology counterpart at UC Medical Center, Sid Khosla, MD, on creating new surgical techniques to improve a patient’s voice.” Dr. Khosla is UC Health’s director of the professional and performance medicine center at UC, associate professor of otolaryngology, and director of the UC Health Voice and Swallowing Center.
Dynamic voice CT scans enable clinicians to look at how different structures may create a voice, and determine the best course of treatment for pediatric patients as their needs change. “We’re performing surgery such as endoscopic posterior cricoid reductions because the scans give us more confidence in our decisions.” This was the topic of Dr. de Alarcon’s Triological Thesis which was recently accepted and will be published in the Laryngoscope. In this procedure, the surgeons remove a section of the rear portion of the voice box to improve voice quality without sacrificing breathing. “This has changed our practice,” Dr. de Alarcon says, “because patient satisfaction is improved when the outcome is a better voice without a ‘big’ surgery which requires lengthy recuperation. With a one or two day hospitalization, and a two-week recuperation, patients feel rewarded with a comparatively low operative risk, shorter recovery, and good voice outcomes.” Young patients with a history of airway reconstruction can now have more efficient voices and louder tones – seemingly small changes, but important for patients who want to be heard.
 Alessandro de Alarcon, MD, MPH
Alessandro de Alarcon, MD, MPH
Associate Professor, UC Department of Otolaryngology -Head & Neck Surgery
Director, Center for Pediatric Voice Disorders
Cincinnati Children’s Hospital Medical Center
University of Cincinnati College of Medicine/UC Health
(513) 636-4335
UCHealth.com

