It’s 7:56 on a crisp autumn morning at University of Cincinnati Medical Center. Physicians and nurses pass through the second floor of the hospital as they prepare for this morning’s surgeries. One physician places a surgical mask on before disappearing behind the doors of an operating room.
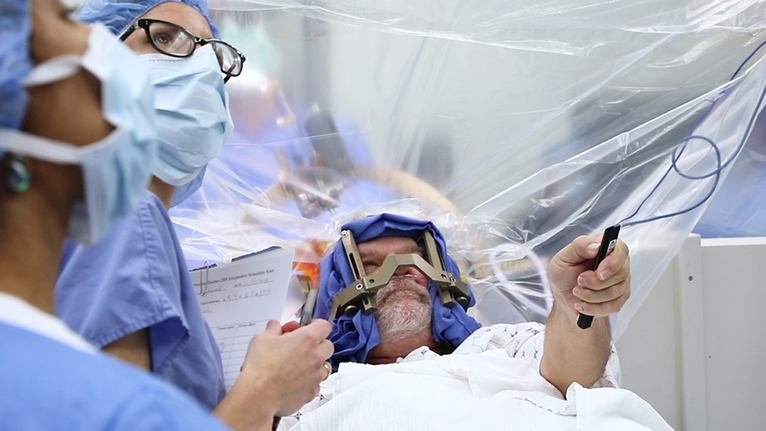
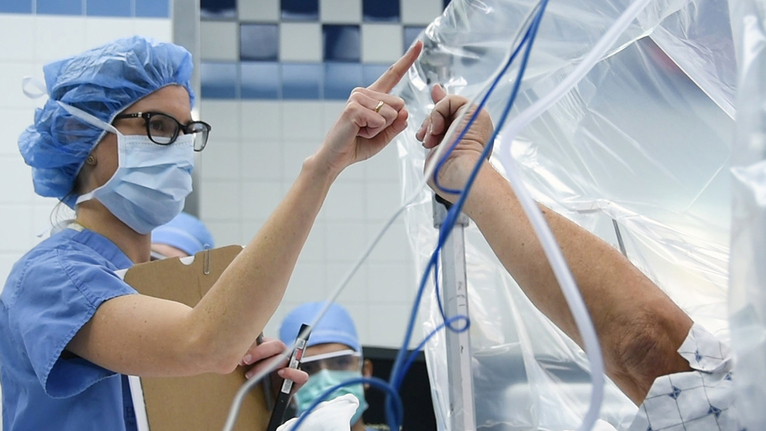
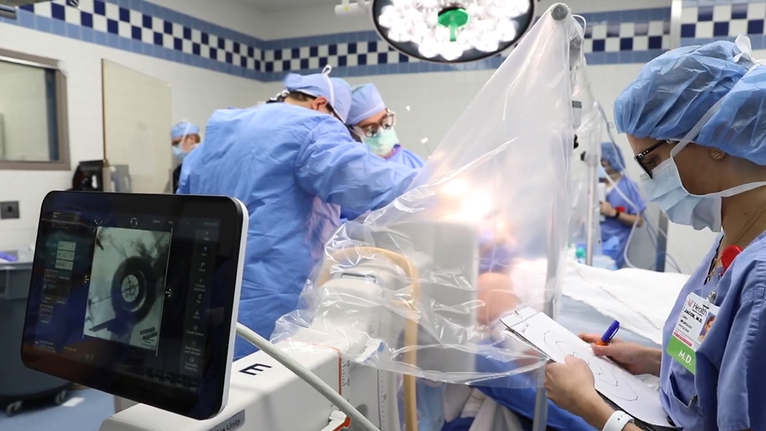
Today, those procedures include deep brain stimulation (DBS) in operating room No. 10 for Richard Crosby, a neurological patient.
Deep brain stimulation surgery involves placing electrodes in the brain that stimulate targeted areas and help control symptoms of neurological disorders including Parkinson’s disease, essential tremor, epilepsy and some forms of dystonia. The electrodes in the brain are connected to a battery in the chest via wires that are underneath the skin.
Electrical impulses are delivered to the brain through the electrodes, similar to how a pacemaker delivers impulses to the heart. Different settings can be programmed into the device based on the patient’s symptoms and can be adjusted over time.
UC Health performs the most DBS surgeries in the region. On average, the team at the UC Gardner Neuroscience Institute performs 40-50 per year.
Richard is a 67-year old patient from Lawrenceburg, Indiana who suffers from essential tremor, causing him to struggle to do even basic things such as eating, reading books or holding tools. He had successful DBS surgery several months ago to help the tremor in his right arm.