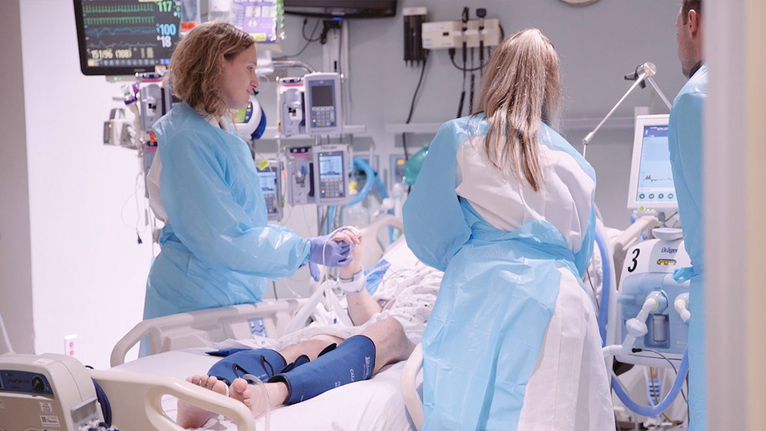
“Hello, good morning! Can you wake up for me for a minute? Can you tell me where you are? UC, that’s right!”
It’s a Tuesday morning in July, and Simona Ferioli, MD, is starting rounds in the neuroscience intensive care unit (NSICU) at the University of Cincinnati Medical Center. Dr. Ferioli, a neurointensivist in the Department of Neurology and with the Neurocritical Care Program of the UC Gardner Neuroscience Institute, is accompanied by an interdisciplinary team as they go room by room to check up on each patient in the 12-bed wing.
By her side is Molly O’Brien, a certified nurse practitioner; neurocritical care fellow Charlie Kircher, MD; Shaun Keegan, a clinical pharmacy specialist for the NSICU; otolaryngology (ENT) resident Michal Trope, MD; and Korey McMillin, RN.*
“Can you open your eyes and look at all these beautiful faces here? How about I help you a little bit?”
Dr. Ferioli explains that sometimes stroke patients lack the ability to open their eyes, but once you help, they are able to keep them open. With some coaxing, the patient opens her eyes.
“Hi there! How many fingers am I holding up here? Very good, OK. Whose hand is this? Look at this hand, this nice nail polish? This hand must be yours. Can you wiggle toes for me? All right.”
Dr. Ferioli notes aloud to the team some sensory neglect on both sides. She also comments that the patient’s arm is swollen from IV fluids, and says to the group, “Let’s keep an eye on this.”