Importance of Ventilators and the Teams that Make Using Them Possible
In the wake of COVID-19, mechanical ventilation has been a consistent topic of conversation. However, there are other instances in which a ventilator may be required for patient care.
Ventilators can be used short-term after surgery. They are used in the intensive care unit (ICU) when patients have pneumonia, sepsis or have experienced major trauma. Patients with neuromuscular diseases, such as amyotrophic lateral sclerosis (ALS) and spinal muscular atrophies (SMA), among others, routinely require long-term mechanical ventilation.
Mechanical ventilation, like any medical intervention, does not come without risks. Complications, including damage to the lung from excessive pressure or volume, a decrease in cardiac function from the positive pressure in the chest, or lung rupture, although rare, can occur.
Some patients require sedation to tolerate ventilation, which can increase their time in the ICU and contribute to delirium or hallucinations. The presence of an endotracheal tube placed through the mouth and into the windpipe can lead to an increased risk of infection.
To help reduce potential complications, the use of a ventilator requires special training and the expertise of a critical care team – an intensivist, a critical care nurse, critical care respiratory therapist and a critical care pharmacist. At UC Health, this multidisciplinary team plays a crucial role. Each subspecialist works together to program, monitor and adjust each ventilator to ensure the best outcome based on the individual care plans determined for their patients.
“Because of the number of highly-trained physicians and the ongoing experience they gain caring for the sickest patients, UC Health has been a leader in the Cincinnati area for critically-ill patients of all causes,” says Evan Ramser, DO, UC Health pulmonary disease physician and assistant professor in the Department of Internal Medicine at the UC College of Medicine. “When special circumstances such as the COVID-19 pandemic sweep over the region, we are uniquely positioned to care for these patients.”
The safety of our critical care teams and clinical staff remains equally as important as the safety of our patients.
“This is unprecedented and worrisome. The disease is easily spread and indiscriminately lethal,” Branson said. “Social distancing has been crucial for limiting the spread of disease and preventing a surge of patients which would strain hospital resources.”
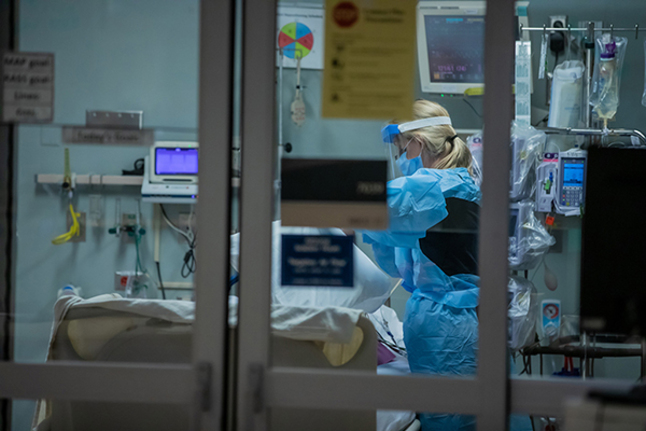
UC Health has implemented strict procedures for donning and doffing, or putting on and taking off PPE, which is critical for everyone’s safety. Our staff is diligent about wearing the proper N95 masks and PPE - face shield, gloves and gown - when entering patient rooms.