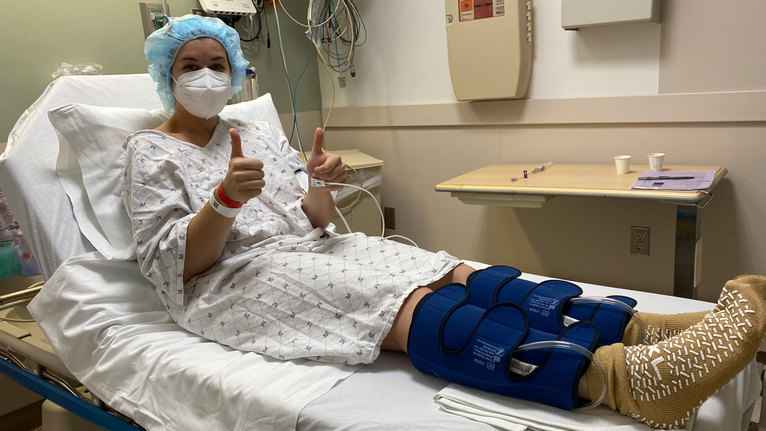
After being first diagnosed with acid reflux by her local ENT specialist, she decided to travel from Indiana to Cincinnati, Ohio, and find answers with the help of internationally respected laryngologist Aaron Friedman, MD, and his voice care team at UC Health.
If you’re into gaming, you’re probably familiar with Minecraft, Sonic the Hedgehog and one of the most played games in the world; League of Legends.
After COVID-19 hit the U.S. in 2020, digital gaming spiked as more people stayed at home, looking to keep themselves occupied and connected to the outside world.
The popularity of gaming is expected to rise, and the success of video and computer games are becoming more competitive than ever in terms of their engaging gameplay, appealing sound effects and music, captivating visuals and a gripping storyline with unforgettable characters.
Many gamers would argue that the relatability and distinguished characters are what separates a mediocre game from a great one—and what brings that character to life is an experienced vocal actor or actress.
MEET ELSPETH EASTMAN, VOICE OF LEAGUE OF LEGENDS’ TRISTANA
Elspeth grew up in rural northern Indiana, enjoying all of the outdoor activities it had to offer. When she wasn’t playing outside or with animals, she was a regular participant in her school’s theater performances.
Fast forward to college, she picked up voice acting as a side hobby and posted her videos on YouTube. Her videos quickly reached hundreds of thousands of viewers, including the attention of creators of the League of Legends. Elspeth landed the role of Tristana, which catapulted her into a full-time career in voice acting, including other major roles in games like Timespinner and Observation.
“I have always been a more theatrical kid,” Elspeth said. “so, I thought, ‘why the heck not?’ It’s fun!”
LOST VOICE AND MISDIAGNOSED
In 2021, however, Elspeth began noticing a difference in her voice.
“My voice had all but disappeared—it was crackly and weak,” she explained.
Elspeth went seeking answers at her local healthcare provider in Indiana where she wasn’t finding any success.
“It was really tough trying to figure out what was wrong,” she recalled. “I was first misdiagnosed as having acid reflux, and I felt I was wasting time with solutions that didn’t work.”
Months went on without improvement, impacting Elspeth’s entire life. Her voice went from crackly and weak to a complete whisper, taking a devasting toll on her health and career.
“I had to take months off of work, and that was beyond stressful,” she explained.
VOCAL CORD POLYP
After many months and no improvement, Elspeth’s partner recommended that she make an appointment with Aaron Friedman, MD, a nationally renowned voice subspecialist at UC Health Performance Voice & Professional Voice.
“My partner lives in Cincinnati and thought that it was worth taking a look, even if it was out of state,” Elspeth said.
After some research, Elspeth recalled that the extensive patient history and peoples’ anecdotes about being truly cared for is what drew her to UC Health.
With just one consultation with Elspeth, Dr. Friedman identified a small polyp on her vocal cords.
“At our Center, we have specialized equipment not commonly available to general ENT physicians, which allows us to record vocal cord vibrations that normally occur very quickly and review them in slow motion to detect even subtle issues,” Dr. Friedman explained. “After a careful examination, we were able to identify a small structural problem on one of Elspeth’s vocal cords. Without this equipment and attention to detail, it is easy to miss a small lesion and otherwise blame a voice disorder on a much more common disease, like acid reflux.”
Polyps typically occur on the edges of the vocal cords, as the edges need to touch in order to vibrate and make the sound that is our voice. If the edges can’t touch completely, people can experience decreased vocal range, sometimes raspiness or breathiness in their tone, and vocal fatigue as the efficiency of their vocal function decreases.
“The vocal cords are one of the fastest moving structures in the body—impacting the pitch of our voices,” Dr. Friedman said. “The average number of vocal cord collisions in a female is about 180-220 times per second, just when speaking. When singing, that number can reach in excess of 1,000 collisions per second. Even when not singing, with nuanced voice actors, such as Elspeth, vocal demands can be incredibly high.”
SURGERY TO REMOVE VOCAL POLYPS
Dr. Friedman recommended surgery on Elspeth’s vocal cords, and, although she was concerned, Elspeth didn’t hesitate for a moment.
Although surgery is a common recommendation for vocal polyps, the amount of surgical precision is crucial.
“The smaller the size of the vocal cord lesion, the more precision you need when operating on the vocal cords, because the margin for error is incredibly low,” explained Dr. Friedman.
“Ideally, a patient needing vocal cord surgery should look for a surgeon with both experience operating on vocal cords, and one who uses the latest techniques and has access to the right instruments. If you create a scar, the patient’s voice could end up being worse than before.”
Dr. Friedman’s expertise is vast—while completing a fellowship in laryngeal surgery at Massachusetts General Hospital Voice Center, affiliated with Harvard University, he was being trained by a world-renowned laryngeal surgeon who has operated on artists such as Adele, Steven Tyler, Sam Smith, and Lionel Richie. Through surgery, Dr. Friedman has also helped save the radio voice of the Chicago Cubs.
He now shares more than a decade’s worth of—right here in Cincinnati.
HEALING VOCAL CORDS AFTER SURGERY USING SPEECH THERAPY
After the post-operative vocal rest period, patients are often enrolled in voice therapy with a speech pathologist to guide the remainder of their recovery.
Elspeth began vocal therapy with speech pathologist Katelyn Reid, CCC-SLP, at UC Health’s Robin T. Cotton and Rocco dal Vera Voice, Swallowing, and Airway Center.
“Katelyn is instrumental in the care and rehabilitation of our voice and swallowing patients,” explained Dr. Friedman. “We have three voice pathologists, all of whom are singers and can understand and guide vocal performers, but they are also incredibly good at relating to and helping anyone with a voice disorder.”
Speech pathology is an incredibly diverse field—from working with patients recovering from traumatic brain injuries on memory issues, patients who have trouble swallowing after a stroke or articulation issues—the list goes on.
“I knew I had a passion to work with voice before I even entered graduate school, so I chose to work in an outpatient clinic with ENT physicians who treat voice, swallowing and airway disorders,” Katelyn said.
“UC Health is quite unique in that we have specialized Speech Language Pathologists (SLPs), meaning that most of us have chosen either voice or swallowing and head and neck cancer care as our primary focus.”
Vocal therapy after polyp removal typically spans the next 4-6 weeks of a patient’s recovery.
“You might think that getting the polyp removed would result in an instant return to normal vocal function—however this is not always the case,” Katelyn explained. “Sometimes even after the polyp is removed, the tension habits created from using the injured voice remain in the body and prevent a person from feeling fully functional ever after they have physically recovered. We can work on releasing this tension with voice therapy exercises.”
After several sessions with Katelyn, Elspeth began seeing and feeling improvements in how she used her voice.
“She gave me a fresh perspective on how I was speaking and where I was holding tension in my voice,” Elspeth remembered.
That tension is the likely cause of what created Elspeth’s vocal polyp in the first place.
Performing and professional voice users project and manipulate their voices on a regular basis—putting an incredible amount of strain on their vocal cords. Occupations like teachers, singers, coaches, attorneys and vocal actors, like Elspeth, are all considered professional voice users. Many of those in these occupations don’t realize the amount of stress and negative impact their voice is undergoing—making vocal health an overlooked priority.
Katelyn helped Elspeth find a comfortable resonant voice, which is important for professional voice users so that they can use their voices in the most efficient and comfortable way.
Elspeth’s profession requires many different vocal extremes, so—thanks to the help of UC Health—found her resting voice—the state in which her voice felt effortless, relaxed and as close as she could get to her natural sound.
“Speaking in your most resonant voice gives you a clear, smooth vocal quality with the least amount of effort,” Katelyn said. “It is beneficial for professional and performing voice users because it decreases vocal fatigue and improves the quality of vocal production so that injury and irritation are less likely to occur. To most people, speaking in their most resonant voice feels very comfortable and effortless.”
“I started to cry from relief. It was a different, stronger tone,” said Elspeth.
It took nearly an entire summer of Elspeth learning how to speak again and rebuilding her voice. This newfound voice wasn’t so far off from her voice pre-surgery, but with the polyp successfully removed by Dr. Friedman and with the help with Katelyn, Elspeth now has the tools and techniques to release the tension on her vocal cords when she isn’t performing.
“It was truly life-changing.”
PRESERVE YOUR VOCAL HEALTH
An injury to your voice isn’t always the career-ending occurrence that many professional voice users fear it to be.
We root for injured sports players to recover however they need to get back on the field or court, and extreme voice users are like vocal athletes and ought to receive the same support.
Here are a few reminders on how to preserve your vocal health:
- Listen to your body and get checked when you notice changes to how your voice is feeling and functioning.
- Remember that voices are vulnerable to inflammation and irritation just like the rest of the body.
- If you experience raspiness or vocal fatigue, make a point to give your voice some breaks during the day and speak less loudly.
- Or if you know what might be affecting your voice because you’re feeling other symptoms—like those of allergies, illness or acid reflux—do what you can to treat those conditions in order to help it recover.
“Be smart about taking care of your instrument, but if something does go wrong, know that there’s a whole team of people at UC Health who understand what you’re going through and are ready to help get you back to feeling your best,” Katelyn said.