Middle Cranial Fossa Surgery Offers a Better Chance for Hearing Preservation
The middle cranial fossa (MCF) approach for operating on acoustic neuromas (ANs) is an excellent treatment option for patients who still have hearing and whose tumors are small- to medium-size (< 2 cm). “MCF has a low risk of intracranial complication, offers excellent facial nerve outcomes and is arguably the best surgical procedure to preserve hearing,” says Ravi N. Samy, MD, chief of the division of otology/neurotology and program director of the neurotology fellowship, University of Cincinnati (UC) Medical Center, and associate professor of otolaryngology, UC College of Medicine. “At UC Medical Center approximately one-third of all AN surgeries are performed using MCF,” he says. Dr. Samy and colleagues operate on patients with tumors up to 20mm in size; “operating on 20mm tumors is not easy, and isn’t done by many other institutions,” he says. According to Dr. Samy, close collaboration with UC Medical Center’s neurosurgeons and intraoperative monitoring team produces exceptional hearing and facial outcomes for AN patients.
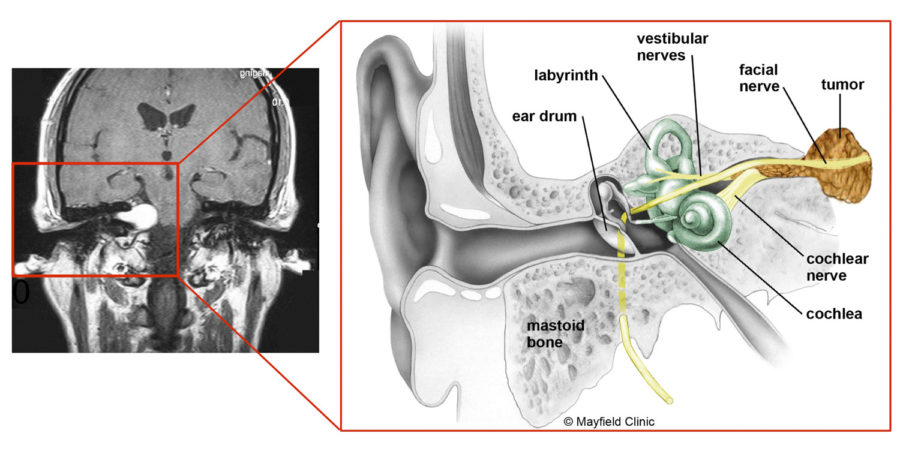
This image shows a benign tumor of the vestibulocochlear nerve (VIII cranial nerve). Image courtesy of Mayfield Clinic
As branches of the vestibulocochlear nerve that lead from the inner ear to the brain directly influence balance and hearing, pressure from an AN can cause hearing loss, ringing in the ear and unsteadiness.
Treatment includes surgical (middle cranial fossa, translabyrinthine, and retrosigmoid/sub-occipital) procedures and nonsurgical options (observation, radiation, and medications such as aspirin). With translabyrinthine surgery, any size tumor can be removed, but hearing loss is complete in the AN ear. In retrosigmoid/sub-occipital surgery, tumor size is not a consideration, but the chance of hearing preservation is arguably not as good as with the MCF approach, according to the findings of Dr. Samy and colleagues. Radiation and medications may be preferable in elderly patients or in persons with smaller tumors; in these cases, surveillance, with repeat scans every 6-12 months, may be recommended. Observation, however, is not without risk (e.g., 5% of tumors are associated with profound hearing loss, tumor growth is not linear, and 50% of tumors grow over three to five years). At UC Medical Center, Dr. Samy and colleagues employ MCF for tumors under 20mm in size (fundus to brainstem with good hearing), unless contraindicated by factors such as advanced physiologic age, significant comorbidities, patient preference, if hearing is present only in the ear afflicted by AN, and if the AN is a neurofibromatosis type 2. Ultimately, tumor size is the most important factor in deciding outcome and guiding treatment choice.
Dr. Samy points out that he cannot know until after surgery that hearing has been preserved. “If the patient has any hearing before surgery, and the nerve can be saved with good blood supply, then a cochlear implant may be an option for single-sided deafness, if the hearing is too poor for hearing aid use,” he says. On average, 55% of patients who have undergone MCF surgery at UC Medical Center have hearing preserved regardless of preoperative hearing status or tumor size.1
UC Medical Center’s forward-looking work in this surgical area includes the possibility of placing a cochlear implant in patients with single-sided deafness, and a dedicated intraoperative monitoring group that is assessing facial function during surgery. This topic will be addressed in a paper that Dr. Samy and his colleagues expect to publish next year.
Reference
1. Quist TS, Givens DJ, Gurgel RK, Chamoun R, Shelton C. Hearing preservation after middle fossa vestibular schwannoma removal: are the results durable? Otolaryngol Head Neck Surg. 2015;152:706-711.
Suggested Reading
Greganov VM, Giordan M, Samii M, Samii A. Diffusion tensor imaging-based fiber tracking for prediction of the position of the facial nerve in relation to large vestibular schwannomas. J Neurosurg. 2011;115:1087-1093.
Lonneville S, Delbrouck C, Renier C, Devriendt D, Massager N. Repeat Gamma Knife surgery for vestibular schwannomas. Surg Neurol Int. 2015;6:153.
Meyer TA, Canty PA, Wilkinson EP, et al. Small acoustic neuromas: surgical outcomes versus observation or radiation. Otol Neuroltol. 2006;27:380-392.
Shuto T, Matsunaga S, Suenaga J. Contralateral hearing disturbance following posterior fossa surgery. Neurol Med Chir. 2011;51:434-437.
 Ravi N. Samy, MD, FACS
Ravi N. Samy, MD, FACS
Neurotologist, University of Cincinnati Gardner Neuroscience Institute
Chief of the Division of Otology/Neurotology
Program Director of the Neurotology Fellowship and Associate Professor of Otolaryngology, University of Cincinnati College of Medicine
Director of the Adult Cochlear and Auditory Brainstem Implantation Program, University of Cincinnati Medical Center
Phone: (513) 558-4143
Email: Ravi.Samy@UC.edu
Connect with Dr. Samy on Doximity
Leave a reply →
