What is refractory epilepsy?
Epilepsy is a common brain condition that causes a person to have seizures—resulting in brain cells experiencing a burst of abnormal electrical activity. When normal connections between nerve cells in the brain are interrupted and depending on the type of seizure, people can experience stiffening of the body, loss of consciousness, breathing problems and confusion.
The goal of epilepsy treatment is to control, stop or reduce how often seizures occur. The most common type of treatment for epilepsy is medication. However, according to David Ficker, MD, UC Health neurologist, director of the epilepsy monitoring units at UC Medical Center and West Chester Hospital, and professor in the Department of Neurology & Rehabilitation Medicine at the University of Cincinnati College of Medicine, about one out of three patients with epilepsy has medication-resistant epilepsy—also known as refractory epilepsy. Refractory epilepsy happens when medications fail to control a patient’s seizures. Another term for refractory epilepsy is medication-resistant epilepsy.
“Refractory epilepsy is first diagnosed in the clinic when we sit down with our patients and intake a careful history, getting a description of the seizure types that they have and their prior treatment response. Once a patient has been identified as having tried two different medications, we diagnose them as having refractory epilepsy,” explained Dr. Ficker.
When diagnosed with refractory epilepsy, patients may need to undergo additional diagnostic testing to determine the exact type of seizure. These methods can help evaluate refractory epilepsy and pinpoint where in the brain the seizures are occurring. This often includes:
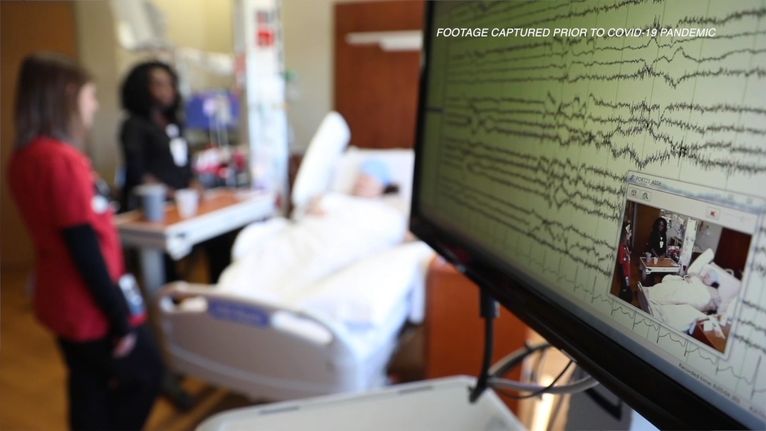
- Video electroencephalogram (EEG) monitoring, or simultaneous video and EEG recordings of a patient’s brain activity and physical behaviors during a seizure. This involves a hospital stay in an epilepsy monitoring unit, which is an inpatient unit specially designed for patients with seizures that helps doctors characterize the seizures, determine the seizure source and guide proper treatment.
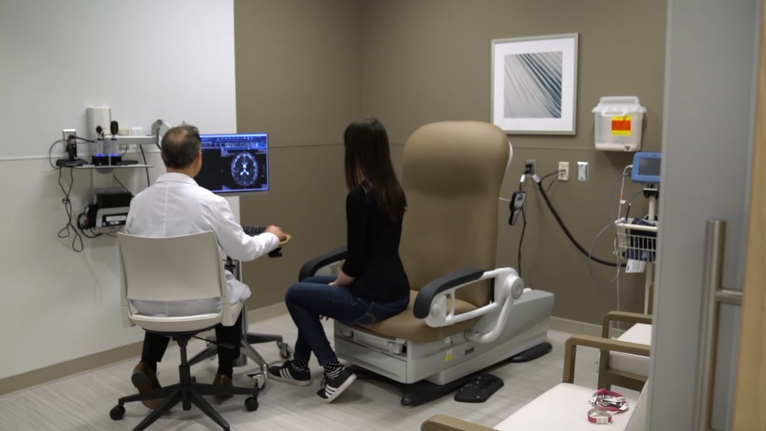
- Advanced imaging including magnetic resonance imaging (MRI), functional MRI, positron emission tomography (PET) and ictal single-photon emission computed tomography (SPECT).
Refractory epilepsy can significantly affect patients’ daily lives and their ability to function well in society. They can face additional stress or anxiety about when or where their next seizure will come and can often struggle to participate at work and school.