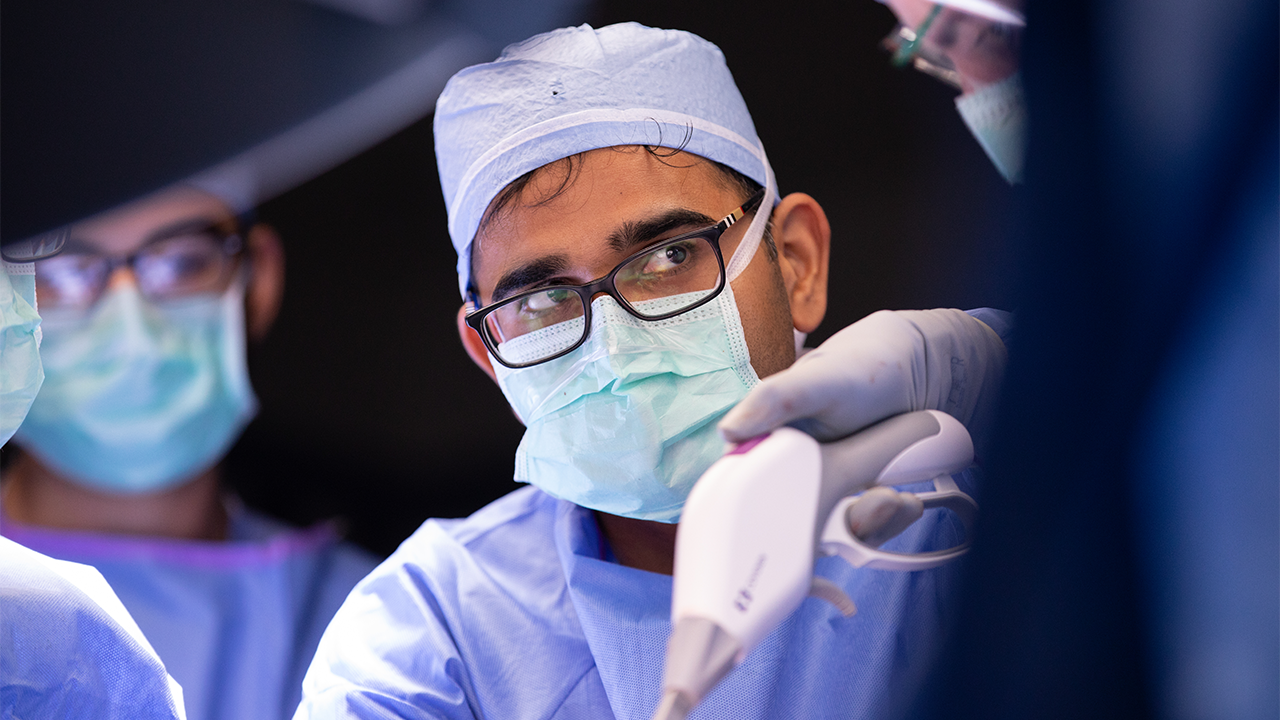
At the time, Randall was in Florida. While out of town, he happened to see a UC Health segment that featured a physician talking about newer prostate cancer treatment options. That doctor happened to be Abhinav Sidana, MD, assistant professor in the Department of Surgery at the UC College of Medicine and director of Urologic Oncology at UC Health. Dr. Sidana is a member of the UC Cancer Center, UC Genitourinary Cancer Center and UC Multidisciplinary Prostate Cancer Clinic.
Unbeknownst to Randall, Dr. Verma and Dr. Sidana work closely together at the UC Multidisciplinary Prostate Cancer Clinic.
“Mr. Cody had been dealing with symptoms for years before I met him in August 2018,” said Dr. Sidana. “His cancer was located in an elusive area of the prostate, but Dr. Verma, a world-renowned radiologist on our team, found an area on the MRI that hadn’t been visible to anyone else. We biopsied it and it came back as cancer.”
Innovative Localized Treatment Options for Prostate Cancer
In the past, prostate cancer patients would be treated with complete removal of the prostate, or radiology/chemotherapy, or a blend of them all.
“In most prostate cancer cases, less than 25% of the prostate is affected by cancer; yet, until recently, we had no way to treat just the cancerous area, so the entire prostate would be removed as an alternative,” said Dr. Sidana.
Now, UC Health offers treatment options for prostate cancer patients with limited involvement of prostate. Instead of having to choose between active cancer surveillance or intrusive surgery with a higher risk of side effects, some men can choose focal therapy treatment.
“With focal therapy, which is similar to a lumpectomy for a breast cancer patient, we’re able to target the cancerous area only, treat it more effectively, and save healthy prostate tissue to limit side effects. We’ve been using the MRI-guided technique to biopsy prostate cancer for a long time, but we’re now using the technique to destroy the cancer,” said Dr. Sidana. “UC Health is the only place in Greater Cincinnati in which such a strategy is employed in taking care of patients with prostate cancer.”
Randall underwent focal cryotherapy with MRI guidance by Dr. Sidana in January 2019.
MRI-Guided Focal Cryotherapy
Focal therapy involves the use of magnetic resonance imaging (MRI) as a guidance tool to find the cancer, and specialized equipment to freeze (cryotherapy) or burn (high intensity focused ultrasound therapy) the cancer, effectively killing the harmful cells.
In the past, Randall’s scans hadn’t revealed one particular cancerous area of his prostate. He lived with the stress of his cancer diagnosis and various treatment options for about five years before finding Dr. Sidana.
Randall’s past biopsies had been done without the aid of an MRI, and his cancer was located in a portion of the prostate where biopsy without MRI wouldn’t be able to spot it.
“Imagine the prostate as a spherical ball. Normally, a biopsy without an MRI only biopsies the sides of that ball, but this patient’s cancer was located at the top of the ball,” said Dr. Sidana. “We only ever biopsy that area if we see a known reason, which we were able to see from our MRI-guided scans.”
On Jan. 29, 2019, Dr. Sidana removed Randall’s cancer via MRI-guided focal laser cryotherapy.
Randall’s recovery was quick. So quick, in fact, that he and his wife, Karen, were able to vacation in Hawaii just six days after the procedure. It was a trip they’d planned for a long time and were thrilled to not have to reschedule.
“I felt like I was finally back to normal, I was up and functioning the day after my procedure,” said Randall. “In Hawaii, we went hiking, climbing mountains, surfing — having fun. It’s amazing the amount of prostate that can be ablated and how resilient the body is.”
A large part of that resilience is credited to Randall’s persistence to do everything in his own power to live healthy and set his immune system up for the best fighting chance. “I took an active role in supporting myself through this process. I’d been researching for years about prostate cancer before I met Dr. Sidana. He treated my cancer AND I also know I’ve given my body the best possible care,” said Randall.
Prior to the procedure at UC Health, Randall would get exhausted easily. He recalls after mowing his lawn he would need to go inside and sleep because he was so drained. Now he not only mows the grass; he removes weeds, prunes trees and completes all the maintenance of his one-and-a-half acres of yard — with energy to spare.
At age 62, Randall is thrilled to continue his active life. “Dr. Sidana moved quickly — he got me in for my MRI and told me that based on my cancer location and past health history, focal cryotherapy was the best option — that made the procedure a no-brainer decision for me,” said Randall. “What I like about Dr. Sidana is that he sees his patients as people first, not as their disease. He’s very professional, yet at the same time warm and personable.”
In 2018, Randall’s PSA number was 18; now it falls between 4-5, which is a healthy score for a naturally enlarged prostate.
“Mr. Cody was one of my first patients to have this procedure, and I’m grateful he had enough faith in someone like myself, telling him about a new treatment which I had just started offering, but I was confident it would help — and he believed in me,” said Dr. Sidana.