UC Health’s Complex Facial Pain Center delivers precise, safe care for trigeminal neuralgia and other facial pain. Led by a nationally recognized expert, our multidisciplinary team pioneered advances—from the curved radiofrequency electrode to early laser use and radiosurgery—and continues to develop gentler, more accurate treatments.
Research and Clinical Trials
Billing and Insurance
Refer a Patient
Research and Clinical Trials
Access the Latest Headache Research and Trials
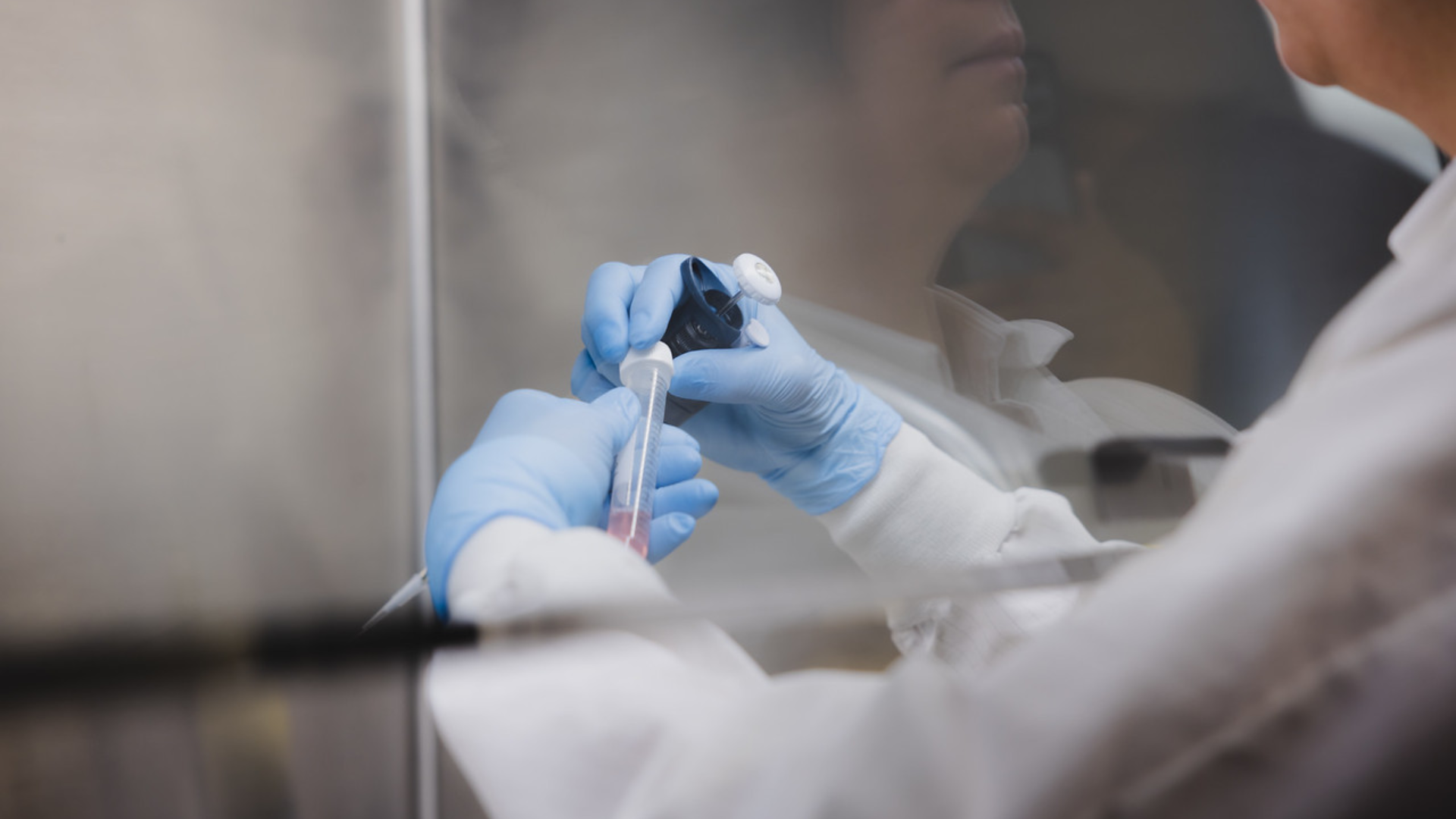
UC Health is the region’s only adult academic medical center, offering access to clinical trials and studies for new therapies, diagnostic tests and ongoing research to improve headache and facial pain care.
Billing and Insurance
Information to Help You Understand Costs and Coverage
Get clear answers about billing, insurance and financial assistance at UC Health. Learn about payment options and get support with understanding your coverage.
Refer a Patient
Information for Healthcare Providers to Refer Patients
Providers can learn how to refer a patient, access our digital toolbox for secure information sharing and coordinate directly with our team for optimal patient care.
Research and Clinical Trials
Research and Clinical Trials
Billing and Insurance
Billing and Insurance
Refer a Patient
Refer a Patient
Our Specialties
Expert Diagnosis and Advanced Therapies for Every Patient
- Conditions We Treat
- Treatments We Offer
{{ letter }}
- {{item.title}} {{item.title}}
- {{item.title}} {{item.title}}
Authoring Breakthroughs
Advanced Care, Research and Teamwork for Better Headache Relief

Featured Benefit
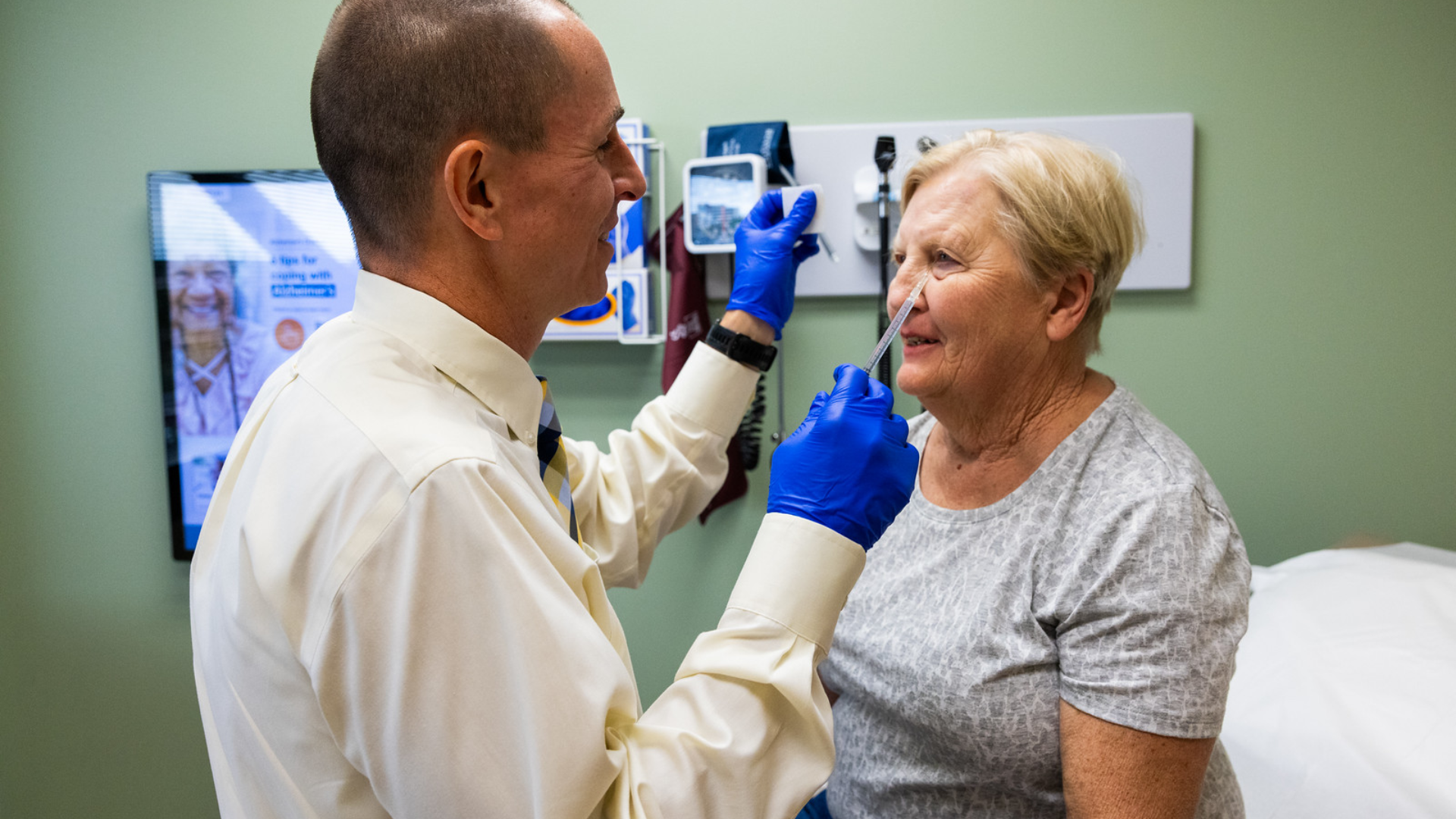
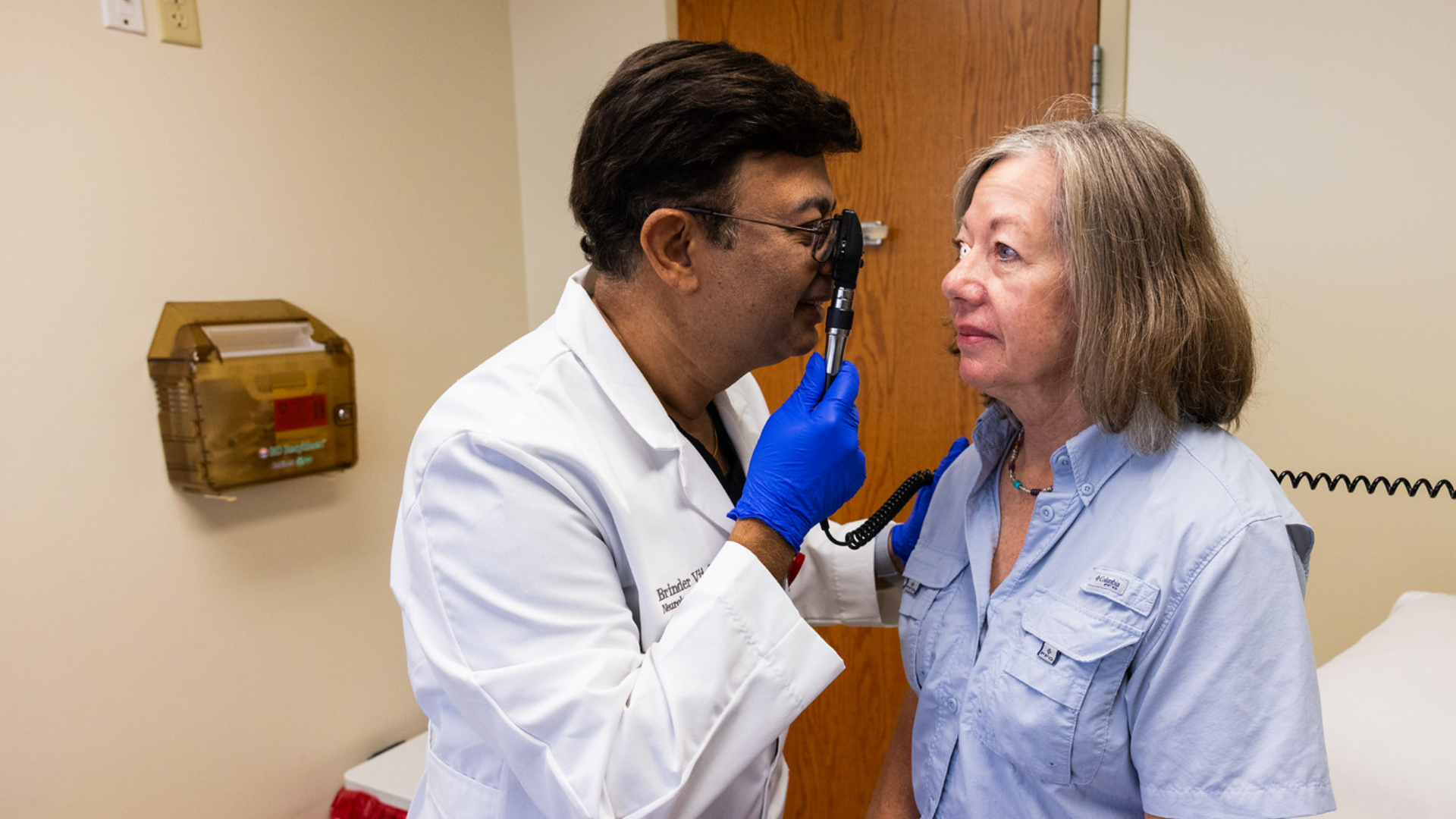
Expert Complex Facial Pain Treatments and Research

Patient Resources
When is a Headache the Sign of Something More?
Whether it’s tension, clusters, migraines or sinus allergies, headaches can tell you a lot about your symptoms.
Our Unique Approach
Patient-First Care You Can Count on
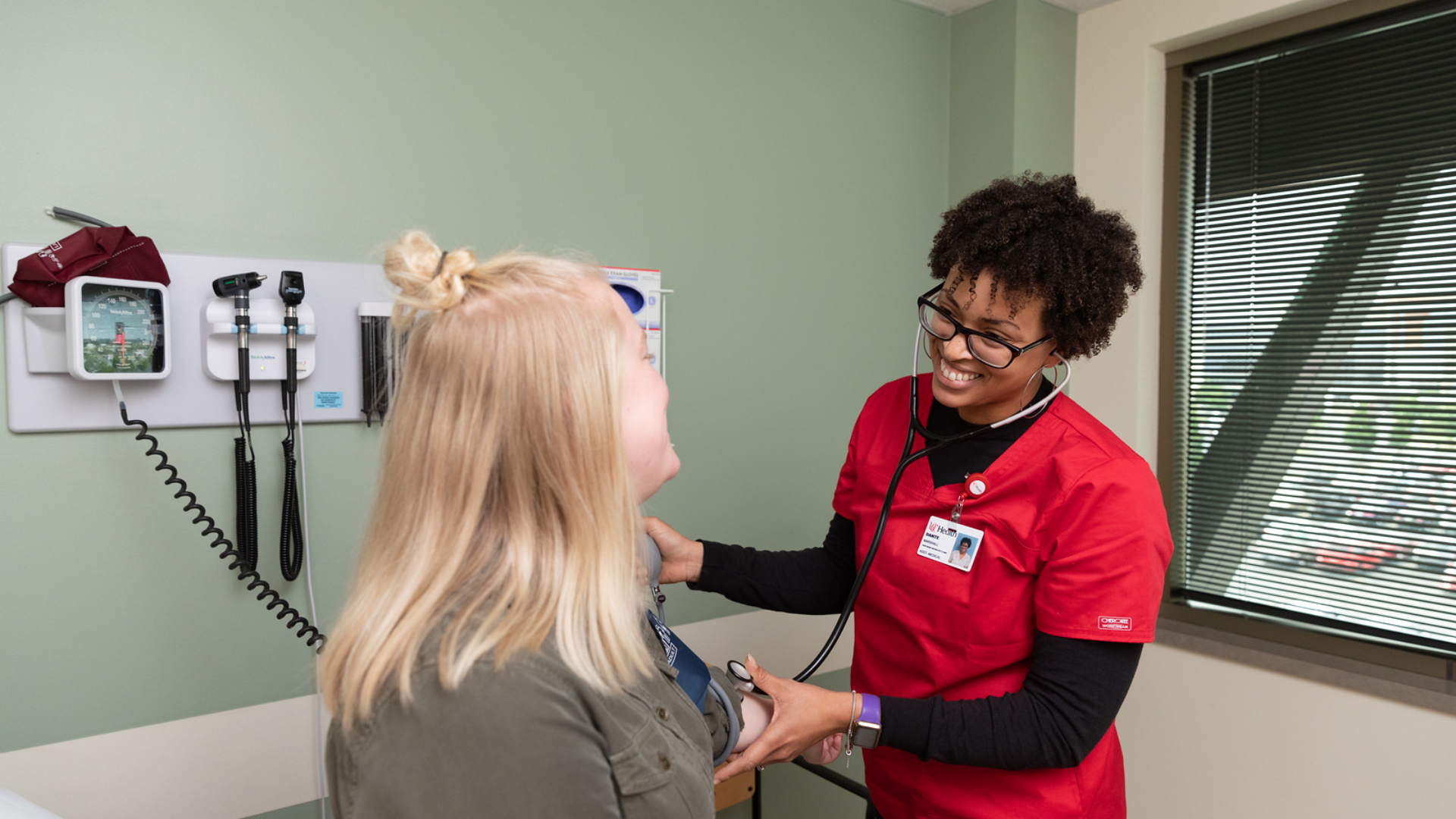
At UC Health, you get individualized treatment from a team committed to your relief. Our collaborative experts deliver care built on research, experience and a passion for helping every person live with less pain.
10,000+
Patients treated each year
10
Headache and facial pain specialists
4
UCNS-certified headache physicians
3
Convenient care locations
How to Contribute
Your Support Advances Headache Care
Your donation to UC Health supports medical research and treatments that change lives. We accept donations to advance medicine and help patients in our community and around the world.

Contact Us
Contact Us
We are here to answer your questions and help you take the next step in your care.