Patient Involvement, Shared Decision-Making Focus of Cystic Fibrosis Foundation “Transformational Change” Quality Improvement Initiative
The Cystic Fibrosis Foundation (CFF) has launched a three-year funding program totaling close to $280,000 called the “Transforming CF Care Through Shared Decision-Making” initiative. It will follow the “Clinical Microsystems” model established by The Dartmouth Institute and currently utilized by the CFF, with a focus on cultivating the improvement capability of frontline staff and leadership development, resulting in more efficient and effective care systems for cystic fibrosis (CF) patients and their families.1 The Adult CF Program at University of Cincinnati Medical Center was recently named as one of only a handful of centers to receive funding under this mechanism.
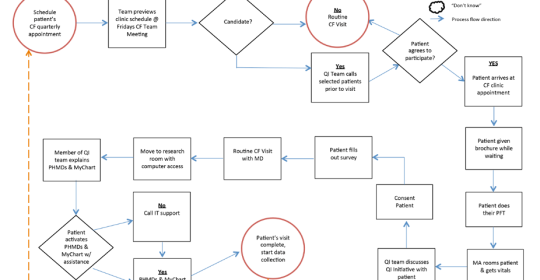
The program at the University of Cincinnati Medical Center, led by Patricia Joseph, MD, Professor of Medicine, will seek to advance three goals: enroll patients in the electronic health record system personal portal called MyChart; engage patients in shared decision-making program regarding treatments, interventions, and barriers to care; and tie outcomes to patient activity, e.g., using a healthcare monitoring device (HMD), such as a FitBit, and Wifi scale to encourage, monitor and measure exercise. A workflow diagram for the study is provided in the schematic.
Joseph has participated in several Quality Improvement programs with the CFF, and last year coached another facility as it implemented its own quality improvement program. One key insight for other facilities embarking on quality improvement initiatives is the importance of providing CF care teams (with patients and families at the center) with information at the point of care delivery, including current care guideline recommendations, patient alerts, clinic reminders and graphical displays of change in key outcomes over time.2 She notes that the CFF has worked closely with Dartmouth to develop a CF-specific program, and was an early proponent of quality improvement as a method of improving patient outcomes. The Clinical Microsystem method stands to benefit numerous CF centers, well beyond the handful who have received CFF grants, as medical centers such as the University of Cincinnati Medical Center will share their procedures and best practices at the conclusion of the trial.
In addition to this quality improvement initiative, the University of Cincinnati Medical Center is one of 23 CF centers to participate in the CFF’s Therapeutics Development Network (TDN), the largest cystic fibrosis clinical trials network in the world.3 The TDN utilizes experts from across the United States to evaluate the safety and effectiveness of new CF therapies through clinical studies, and provides a central repository to streamline research so that patients can benefit from treatment advances as soon as possible.3 Currently, the University of Cincinnati Medical Center is participating in seven clinical trials for fast-tracked pharmaceutical agents.
While research grants to conduct clinical trials are common, funding to implement quality improvement initiatives is not. Joseph states, “This is a unique grant for the CFF. They’re looking for big ideas, and trying to get adult patients interested and involved in their own care is a big idea.”
 Patricia Joseph, MD
Patricia Joseph, MD
Professor of Medicine, Department of Internal Medicine
University of Cincinnati Medical Center
Medical School: University of Tennessee
(513) 558-4826
josephpm@ucmail.uc.edu


