Recent Findings from a French General Practice Population Highlight Statin Underutilization in Patients with Severely Elevated Cardiovascular Risk
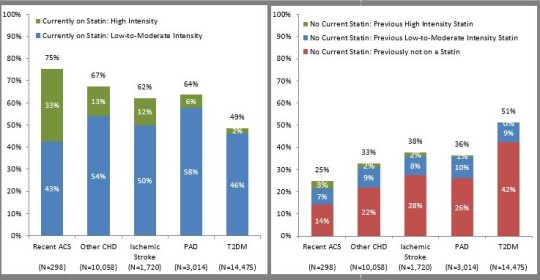
LMT by hierarchical CV risk categories2*
* Classifies each individual into one of five mutually-exclusive, hierarchical categories based on presumed risk, in the following order: recent ACS, other CHD, ischemic stroke, PAD and T2DM.
Although the most current European Society of Cardiology guidelines recommend that patients at very high cardiovascular risk maintain a low-density lipoprotein cholesterol (LDL-C) of <70 mg/dL (<1.8 mmol/L), a recent study demonstrated that most patients from a French population do not meet this goal.1 One of the main causes is the chronic and widespread underuse of statin medications, especially at the appropriate doses, according to Dylan Steen, MD, MS, Director of Clinical Trials and Population Health Research at University of Cincinnati Division of Cardiovascular Health and Disease. Along with a French colleague, he presented the poster, “Statin Utilization and Low-Density Lipoprotein Cholesterol Goal Attainment in Patients at Very High Cardiovascular Risk: Insights from a French General Practice Population” at the European Society of Cardiology Congress in London in 2015.
The research studied patients from 2013 followed by general practitioners in France using electronic health records (EHR). The analysis cohort included 30,000 patients with at least one of the following indications for statin therapy: recent acute coronary syndrome (ACS within one year), stable coronary heart disease (CHD), ischemic stroke, peripheral arterial disease (PAD) and/or type II diabetes mellitus (DMII.)2 At the time of analysis, 43% of the patients received no statin therapy. Only 7% of the study cohort was treated with the most effective statins (high-intensity), despite their proven history of safety and efficacy.2 Data revealed that underutilization of statins was chronic, suggesting that providers were not reassessing whether their patients could be started on a statin.
Steen believes these suboptimal figures stem from several sources. Contrary to data from multiple, large, randomized, placebo-controlled trials, providers frequently attribute muscular side effects such as pain, stiffness, or weakness to statins. Another significant issue that affects medications across the spectrum of cardiovascular diseases is suboptimal patient adherence. Patients find it difficult to understand the importance of taking daily medications for asymptomatic conditions, especially when added to the burden of taking many other medications. Says Steen, “The non-adherence literature clearly demonstrates that the more pills a patient is asked to take, the lower the chances he or she will take any one of them. Each medicine that gets added makes it more likely that the patient will stop or only intermittently take the others. Clinicians can improve adherence by eliminating less important medications, educating patients, and helping patients prioritize which prescriptions are truly important – and for someone with a history of atherosclerotic disease, a statin is likely the most important medicine.”
Improving the utilization of statins is especially important as most experts believe the LDL-C goal should be lowered from 70 mg/dL to about 50mg/dL. Says Steen, “Lowering LDL-C is still the most effective and safest treatment strategy in the fight against atherosclerotic CV disease. New research indicates patients would benefit from even lower levels of LDL-C. These data come from the IMProved Reduction of Outcomes: Vytorin Efficacy International Trial (IMPROVE-IT) which studied ezetimibe (lowers LDL-C 22%), as well as new analyses from trials of statins and a novel class of potent LDL-C lowering drugs called PCSK9 inhibitors.”3 In the French cohort, only 30% of those taking high-intensity statins achieved an LDL-C < 70mg/dL, thus it seems clear that even in the setting of high-intensity statin use, ezetimibe and potentially other medications will be needed in many patients to achieve an even lower goal. The PCSK9 inhibitors, while demonstrating promising early findings, are still undergoing large outcomes studies.
References: 1. Catapano A, Reiner Z, De Backer G, Graham I, Taskinen M-R, Wiklund O et al. ESC/EAS Guidelines for the management of dyslipidaemias. The Task Force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and the European Atherosclerosis Society (EAS). Atherosclerosis. July 2011;Volume 217(S1):1–44. 2. Ferrieres J, Steen D, Sanchez RJ, Chin J, Gorcyca K and Khan I. Statin utilization and low-density lipoprotein cholesterol goal attainment in patients at very high cardiovascular risk: insights from a French general practice population. 3. http://www.acc.org/latest-in-cardiology/clinical-trials/2014/11/18/16/25/improve-it. Accessed October 28, 2015.

Dylan L. Steen MD, MS
Director of Clinical Trials and Population Health Research
Division of CV Health and Disease
Phone: (513) 558-6573
E-mail: Dylan.Steen@uc.edu
Connect with Dylan Steen, MD on Doximity

