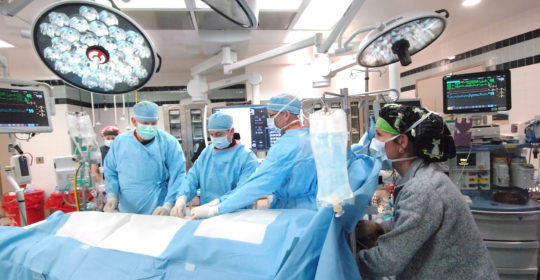
Treating Cardiogenic Shock: A Multidisciplinary Team Approach Achieves Better Outcomes
University of Cincinnati (UC) Medical Center has instituted a team approach for the treatment of acute cardiogenic shock, setting it apart from most medical centers and providing a critical advantage for such acutely ill patients. “With our growing STEMI volume, the team identified the need to provide early intervention for the patient in acute cardiogenic shock, much like the ‘golden hour’ for trauma patients,” says Suzanne Bennett, MD, director of anesthesiology critical care and co-founder of the program. “When a patient meets specific criteria for refractory cardiogenic shock, the shock team allows the interventional cardiologist to focus on revascularization while the critical care anesthesiologist provides hemodynamic and respiratory support to prevent the patient’s further deterioration.”
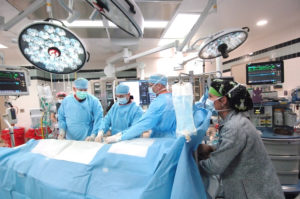
The cardiogenic shock team, from right: Suzanne Bennett, MD, Trauma and Critical Care Anesthesiology Division Leader;
David Feldman, MD, PhD, Director Advanced Myocardial and Circulatory Services;
Alan Simeone, MD, Cardiac Surgery, Trauma and Critical Care, Cardiopulmonary Transplantation and Mechanical Circulatory Support;
Timothy Smith, MD, Cardiovascular Critical Care, Interventional Cardiology; Jessica Gummow, CCP, chief perfusionist
The team, led by David Feldman, MD, PhD, director of clinical services, and Louis B. Louis, IV, MD, FACS, chief of cardiac surgery, has developed selection algorithms and criteria that enable it to respond in a controlled fashion resulting in optimal patient outcomes.1 The decision to proceed onto advanced mechanical support is not made in isolation, Dr. Feldman says, and the majority of the physician team members must agree prior to the initiation of mechanical circulatory support. “UC Medical Center is one of very few medical centers to have a multidisciplinary shock team to treat patients in acute cardiogenic shock, which provides early patient optimization and likely improves patient survival,” he says.
Extracorporeal membrane oxygenation (ECMO) is the foundation for mechanical circulatory support in the acute shock setting at UC Medical Center. In the modern era, using ECMO for acute shock is associated with a 41-70% survival,2,3 compared with a less than 20-30% survival without intervention.3,4 In addition to ECMO, there are other advanced mechanical circulatory support options available to the UC Medical Center shock team, which decides in a multidisciplinary fashion which modality is best for the individual patient. The field of temporary cardiac circulatory support devices is growing rapidly, and programs must stay on the cutting edge to be able to provide excellent, quality care to this gravely ill patient population.
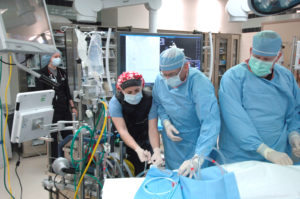
Dr. Smith is preparing to insert the venous cannula for the circuit while Jessica Gummow and Dr. Simeone prepare the circuit to be attached to the cannula.
Once safely on mechanical circulatory support, the patient is transferred to the Cardiovascular Intensive Care Unit (CVICU) where he/she will be managed by a multidisciplinary team who will determine whether the patient can recover cardiac function, or is a candidate for more advanced therapies, such as a long-term implantable left ventricular assist device (LVAD), and/or eventual heart transplantation. [Related: ECMO Is a Bridge to Transplantation for A 35-Year-Old Man with Chest Pain.] “By arresting the shock syndrome, and preventing organ damage, we leave the patient with more options for long-term survival,” says Dr. Louis.
The rapid deployment of a multidisciplinary team to provide immediate cardiovascular support for patients who have life-threatening shock is one more way UC Medical Center is demonstrating its commitment to advancing the field of cardiovascular medicine, and providing a resource for the community in a collaborative fashion, leveraging the expertise and professionalism of its clinician scientists.
References and Suggested Reading:
- Early ECMO referral for better patient prognosis. Cardiovascular Insights. Available at https://uchealth.com/cardiovascular-insights/early-ecmo-referral-for-better-patient-prognosis/. Accessed March 23, 2016.
- Extracorporeal Life Support Organization. Available at www.elso.org. Accessed March 23, 2016.
- Sheu JJ, Tsai TH, Lee FY, et al. Early extracorporeal membrane oxygenator-assisted primary percutaneous coronary intervention improved 30-day clinical outcomes in patients with ST-segment elevation myocardial infarction complicated with profound cardiogenic shock. Crit Care Med 2010 (38)9: 1810-1817.
- Goldberg RJ, Gore JM, Alpert JS, et al. Cardiogenic shock after acute myocardial infarction. Incidence and mortality from a community-wide perspective, 1975-1988. N Engl J Med 1991; 325:1117.
Feldman D, Pamboukian SV, Teuteberg JJ, co-chairs. ISHLT Guidelines. The 2013 International Society for Heart and Lung Transplantation Guidelines for mechanical circulatory support: Executive summary. J Heart Lung Transplant. 2013;32:157-187.
LeGuen M, Nicolas-Robin A, Carreira S, et al. Extracorporeal life support following out-of-hospital refractory cardiac arrest. Crit Care. 2011;15(R29):1-9.
Muller G, Flecher E, Lebreton G, et al. The ENCOURAGE mortality risk score and analysis of long-term outcomes after VA-ECMO for acute myocardial infarction with cardiogenic shock. Intensive Care Med. 2016;42:370-378.
Stretch R, Sauer CM, Yuh DD, Bonde P. National trends in the utilization of short-term mechanical circulatory support. J Am Coll Cardiol. 2014;64(14):1407-1415.
 Suzanne Bennett, MD
Suzanne Bennett, MD
Assistant Professor of Anesthesia
(513) 558-4194
BENNETSZ@ucmail.uc.edu
Connect with Suzanne Bennett, MD on Doximity
Leave a reply →
